Nursing Narratives: A Day in the Life of a Labor and Delivery Nurse

Today’s post is First in our series, Nursing Narratives.
Nurse Paralegal USA staff Nancy Saucier, R.N. relates her first-hand account of labor and delivery involving a cord prolapse.
On a day without emergencies …
The typical day would start with the staff nurses for the day sitting down together and getting a report from the night nurses on all the patients on the floor. The day nurses would decide among themselves how the patient load would be divided up. The patient load would depend on the acuity of the patient. For instance, if the patient was to have a vaginal delivery, the nurse might have 1-3 patients. If the patient were in active labor, the nurse might have 1-2 patients, depending on staffing.
Once the patients were assigned, each nurse would visit her laboring patients and introduce herself. She would provide ice chips if needed. She would then assess the patient, including vital signs and fetal heart monitor strips. The nurse might also turn up Pitocin to assist in the progression of labor if necessary. Additional duties of a labor and delivery nurse might include:
- Helping in a D&C after a miscarriage.
- Assisting with manual manipulation of a baby in breech presentation (also known as external version)
- Helping during placement of cerclage (surgical closure of the cervix to prevent premature birth)
- Perform non-stress tests to monitor the fetus
- Perform a contraction stress test to determine if the baby can tolerate the stress of contractions during labor
Nancy’s unit routinely performed multiple c-sections in a single day. The night shift would usually start iv’s and get lab work before the procedure. Management assigned one day nurse – the circulating nurse – to assist solely with c-sections. Sometimes there would be one c section at 7:30 a.m. and one at noon. Or, on a busy day, there might be multiple c sections in a row.
There might be a c-section “waiting in the wings” when the circulating nurse came in that morning. Routine duties of the circulating nurse would include:
- Documentation of the procedure
- Getting the patient set up on monitors
- Setting up a catheter for an epidural (spinal injection of pain medicine)
- Handing surgical tools and instruments to the physician or surgical tech performing the procedure and assisting with the care of the baby once delivered.
The entire c section “team” would include two doctors, a scrub tech who handled sterile equipment, and the circulating nurse.
Once the c-section was complete, the focus would be to get the baby stabilized. Then the mother would go to recovery accompanied by the circulating nurse. The nurse would stay in recovery with the mother until she was moved out to the post-partum floor. Another nurse would stay with the patient in recovery if there were multiple c sections to be performed.
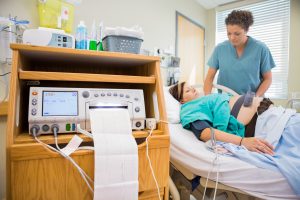 Emergencies
Emergencies
We asked Nancy what would constitute a need for an emergency c section. Although the general perception is that a breech presentation (feet first instead of headfirst) is a significant indicator for an emergency c section, this is not necessarily an emergency. If the mother had good prenatal care, the condition would have been identified weeks earlier. The mother would come in and get an epidural and be ready for delivery.
On the other hand, a baby in distress or a mother with uncontrolled high blood pressure and seizures were indications for an emergency c-section. Nancy stated, “Emergency c sections usually employ the use of general anesthesia as opposed to an epidural. The 10 minutes required for insertion of an epidural catheter is too much time to sacrifice in an urgent situation.”
On occasion, a patient who had been stable throughout her pregnancy would come in for a scheduled c-section and suddenly deteriorate. The pre-op fetal monitor might register the baby’s heart rate at a 50 (normal for a fetus is 120-160). The medical staff would perform an emergency c-section. However, the distressed baby might not survive.
Nancy also witnessed a tragic event when a laboring patient on the way to the hospital was in a car accident. The accident victim suffered multiple broken bones and placental abruption: the baby did not survive.
Placental abruption and cord prolapse – two of the terrifying things that can happen with unstable patients – are the worst nightmares for a labor and delivery nurse. The placenta that nourishes the fetus separates from the uterus in placental abruption. It can cause profuse bleeding, and the baby can die fast. The baby is pressing down on the umbilical cord which delivers nutrients and oxygen, depressing his circulation, in cord prolapse. If the condition is not corrected immediately, the baby will be stillborn.
The first-hand account of a cord prolapse
Nancy took care of one patient during a cord prolapse. To complicate matters, the individual was disabled, had palsy, and was hysterical. The unit was packed with patients that day, and the nursing staff was stretched thin. Nancy was charge nurse. The nurse assigned to the patient came to her in tears. The patient had screamed every time she touched her. She could not get an accurate heart rate on the baby. Nancy called the patient’s doctor, and she relieved the nurse assigned to the patient.
The physician came to the patient’s room, did a vaginal exam, and ruptured the amniotic sack. He immediately felt the umbilical cord descend into the vagina.
Someone must keep their hand in the mother’s vagina when cord prolapse occurs. This action holds the baby’s head off the umbilical cord to prevent the circulation from being cut off. Nancy climbed onto the bed with the patient. She inserted her hand into the vagina so that the physician could withdraw his hand to scrub for surgery. She rode down to the operating room on the hospital bed with the patient while continuing to keep the baby’s head from descending onto the cord, with the patient screaming hysterically. The staff moved the patient to the operating room table with Nancy continuing to hold the baby’s head. The patient was prepped and draped. Nancy stayed with the patient under the drapes. She was not able to remove her hand until the physician made the incisions for the c-section and delivered the baby. Happily, the baby was stable with no impairment to his circulation. Mom, Dad, and baby were all thrilled once the ordeal was over!

Do you have questions concerning a labor and delivery case?
Our NPUSA nurses would love to help you decipher the medical jargon and illuminate case events with a comprehensive medical records summary. Call 504 236-5435 or contact [email protected] at any time with questions.