The Role of Fetal Heart Monitoring in Identifying the Need for a C-Section
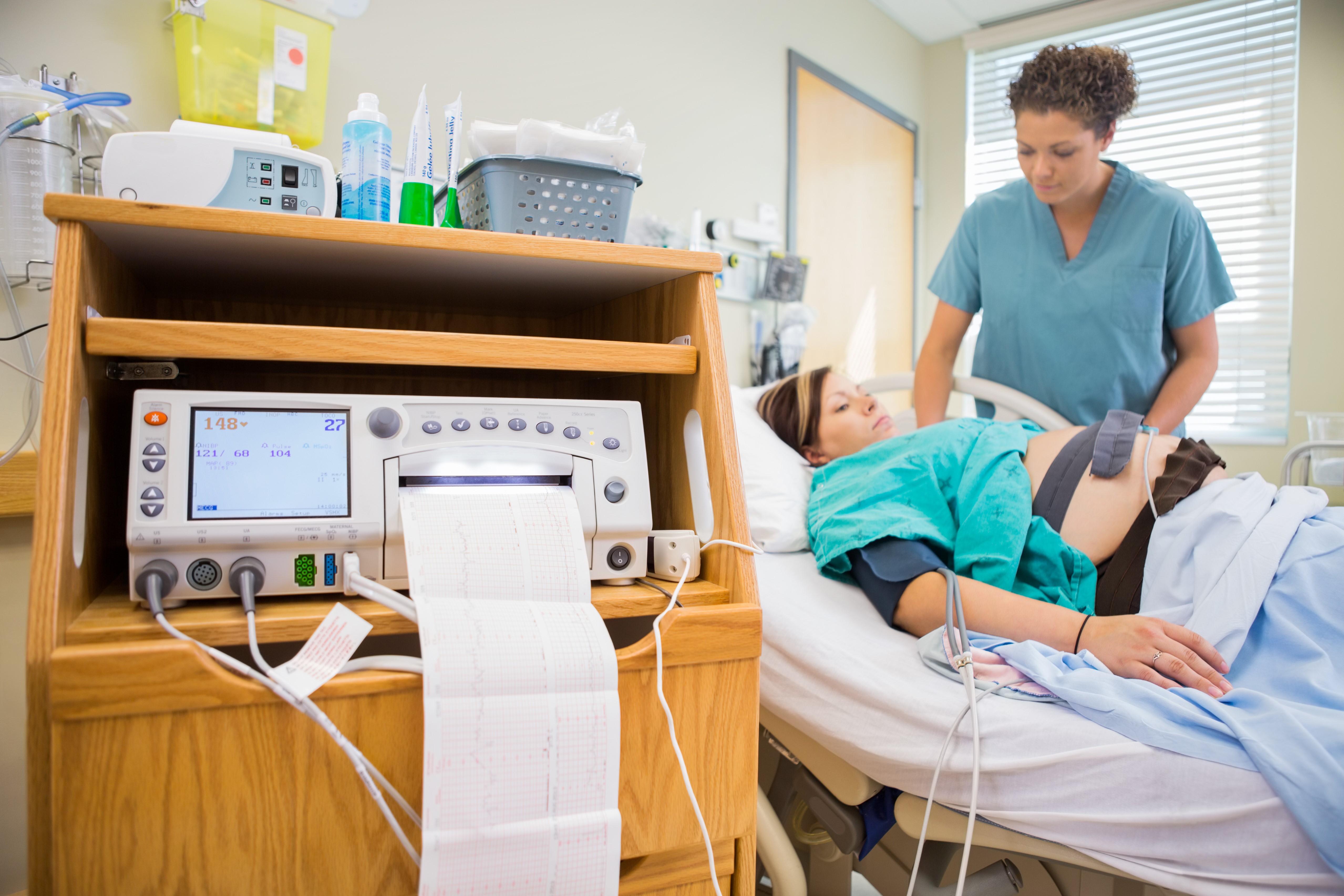
The clinical practice of auscultating fetal heart tones began in 1818 when a Swiss surgeon reported hearing the fetal heart rate by placing his ear against a pregnant woman’s abdomen. In 1888, an American physician, Dr. Killian, suggested that Fetal Heart Rate information could be used to identify the need for intervention for fetal distress. FHR was first introduced to the public by Yale in 1958 but did not become widely used in obstetric care until the 1970’s. Since then, it has become an accepted standard in the management of ob gyn patients who are in labor and close to delivery.
There are external and internal fetal monitors. External monitors (also known as ultrasound transducers) are usually composed of a belt with a doppler ultrasound that is strapped to the pregnant woman’s belly. Internal monitors consist of an electrode attached to the fetal scalp. The fetal membranes must be ruptured to apply an internal monitor. External monitoring is subject to loss of signal related to maternal positioning, fetal positioning, maternal body fat.
A normal fetal heart rate range is 115-150 beats per minute (much faster than a normal adult heart rate). A slow heart rate, or bradycardia, may indicate the baby is not getting enough oxygen delivery to the brain. A fast heart rate, or tachycardia, may indicate oxygen deprivation. There is an acceptable range of acceleration and deceleration – or speeding up and slowing down – of fetal heart rates during contractions and labor. “Variable deceleration” or “late deceleration”, however, may be signs that the baby is not doing well. Variable decelerations are irregular dips in the fetal heart rate that may indicate cord compression, a potentially dangerous condition for the baby. Late decelerations begin with a uterine contraction and continue for too long after the contraction has resolved. This may be a sign that the baby is distressed.
Obstetricians and nurses must carefully review fetal monitor strips throughout labor and delivery to ensure fetal heart tones are reassuring and the baby is getting enough oxygen. If non-reassuring conditions occur, appropriate and timely actions must be taken. Generally, nursing interventions are attempted first to restore normal oxygenation to the baby. These include the administration of supplemental oxygen, changes in maternal position, increasing intravenous fluids, and the administration of medications that subdue contractions and maximize placental blood flow. If fetal heart tones remain non-reassuring despite nursing interventions, the fetus should be delivered by emergency cesarean section. Emergency cesarean section should be performed within 5 to 30 minutes depending on the circumstances.
It is hard to help a distressed baby in the uterus: a C-section is the best and fastest way to handle a baby in distress. Resuscitation, oxygen, fluids, and other lifesaving interventions may be quickly administered once the baby is born.
What to look for in the medical records:
- Fetal heart monitoring strips
- Maternal vital signs
- Maternal Oxygen saturation
- Maternal blood sugar
- Types of medications used during labor such as Pitocin
- Dose and rate of infusion of Pitocin. Sometimes the rate of infusion is stopped, slowed down or increased according to the pattern of contractions.
- Pharmacy records showing amounts of Pitocin charged to the patient chart
- Volume and rate of intravenous fluids administered to the mother
- Documentation on maternal anxiety which could create abnormal breathing patterns that would impact the fetus
- Anesthesia records regarding epidural administration and any effects on the mother
http://www.aafp.org/afp/1999/0501/p2487.html
https://www.abclawcenters.com/practice-areas/prenatal-birth-injuries/labor-and-delivery-complications-and-errors/improper-fetal-monitoring/
http://perifacts.eu/cases/Case_680_Fetal_Heart_Rate_Interpretation.php